Epilepsy in dogs and cats
What is epilepsy?
Epilepsy is a general term for neurological disorders that bring on sudden and repeated seizures. A seizure, also known as a ‘fit’, is a temporary and involuntary disturbance of normal brain function that is usually accompanied by uncontrollable muscle activity. In simple terms, a seizure is an abnormal, uncontrolled burst of electrical activity in the brain.
Epilepsy is characterised by a pattern of repeated seizures over time. These are usually irregular episodes that start and finish very suddenly, that appear very similar each time and have a repetitive clinical pattern.
Epilepsy is more common in dogs than in cats. In both animals, seizures often occur during rest or sleep, either at night or early morning. Most seizures last between 5 and 60 seconds but some may be as long as several minutes. They can occur with or without a loss of consciousness. Typically, the animal will stiffen and fall on its side, where it will salivate, chew at its mouth, paddle its limbs, release its bladder or bowels and/or cry out. After a seizure, the animal may appear confused and disoriented, and recovery can take from a few minutes to up to 24 hours.
There are several types of epileptic seizures:
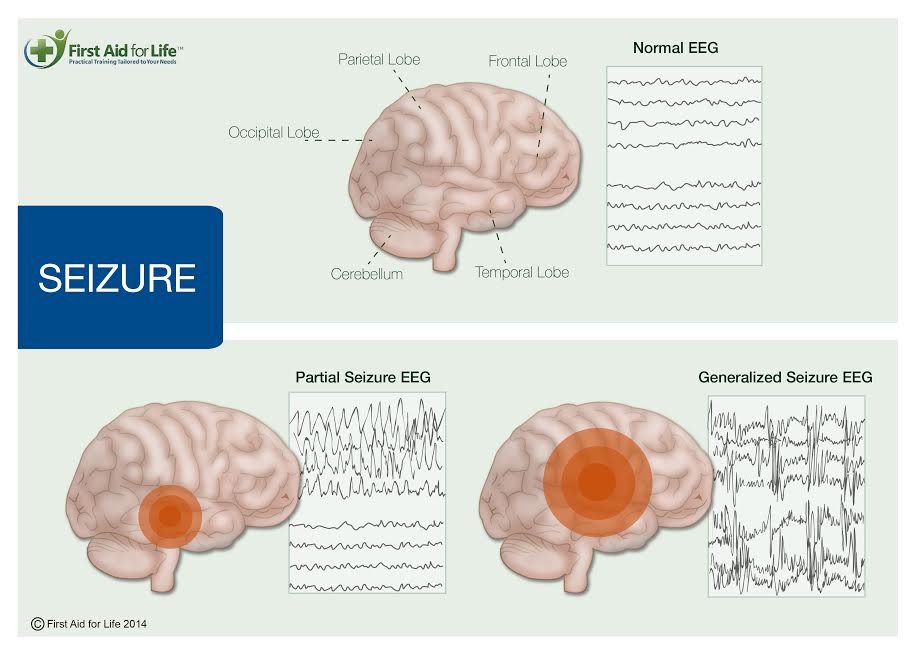
Grand mal or generalised seizure
- The most common type
- Abnormal electrical activity occurs throughout the brain
- The entire body is affected – all the limbs may jerk and twitch
- Can cause loss of consciousness and convulsions
- Last for a few seconds to a few minutes
Focal or partial seizure
- Abnormal electrical activity occurs in a section of the brain
- Can cause unusual movements in one limb or on one side or area of the body, for example, facial twitches or head shaking
- May last only a few seconds
Focal seizure evolving into a generalised seizure
- This is the most common seizure pattern occurring in dogs
- The initial focal seizure may be very short and difficult to detect
- The secondary generalised seizure follows very rapidly
Complex partial seizure or psychomotor seizure
- More difficult to recognise as there are no typical convulsions
- Characterised by unusual behaviour that lasts a couple of minutes, for example, attacking an imaginary object, frenzied barking or staring into space
- Different from odd behaviour in that the animal repeats the same behaviour with every seizure
Symptoms of epilepsy in dogs and cats
Symptoms can vary depending on the underlying cause and the severity of the seizures. Non-specific signs may include anorexia, lethargy or unusual behaviour. Some animals may appear dazed and disorientated before a seizure, or exhibit subtle signs such as crying, clinginess, wild changes in behaviour, pacing and attention seeking.
During the seizure itself, some of the typical symptoms include:
- Muscle twitching
- Jerking or paddling motions of the legs
- Collapsing or falling to the side
- Rigid extension (stiffening) of the legs
- Involuntary vocalisation/calling out
- Foaming at the mouth
- Drooling
- Involuntary urination and/or defecation
- Tongue chewing or biting
- Mouth bleeding, from biting
- Loss of consciousness
- Loss of breathing
Causes of epilepsy in dogs and cats
Many different underlying diseases and other contributing factors can cause seizures. Generally, epilepsy can be classified as ‘structural’, where an underlying cause within the brain can be identified, or ‘idiopathic’, where no underlying cause can be identified.
A ‘reactive seizure’ usually occurs in response to a temporary disturbance in brain function, which may be caused by metabolic changes or poisoning and is reversible if the cause can be treated or eliminated.
Causes of structural epilepsy
In cases of structural epilepsy, an underlying cause can be found in the animal’s brain. These may include problems with blood supply in the brain, such as obstructions, as well as bleeding, inflammation, infection, trauma, developmental problems, brain tumours and degenerative brain diseases. Metabolic disorders affecting the brain can also lead to structural changes in the brain and lead to seizures.
Causes of idiopathic epilepsy
In many cases there is no identifiable underlying cause for the seizures and the condition is classified as idiopathic epilepsy. In some dog breeds there is a clear genetic and familial predisposition, with the condition manifesting in certain family lines. Idiopathic epilepsy usually affects young to middle age dogs (6 months to 6 years old) and it appears more prevalent in male dogs. Without treatment, seizures will become more severe and frequent.
Susceptible breeds include Border Collies, Australian Shepherds, Labrador Retrievers, Beagles, Belgian Tervurens, Collies, Vizslas, Shetland Sheepdogs, Keeshond, Golden Retrievers and German Shepherds.

Cat and dog seizures have many other possible causal and contributing factors, including:
- Kidney disorders / disease
- Liver disorders / disease
- Ingesting poisons or toxins, like antifreeze, lead or even chocolate
- Fevers and hyperthermia
- Congenital defects
- High blood glucose (sugar) levels
- Low oxygen levels in the blood (could be caused by anaemia, breathing issues or heart problems)
- Certain medications
- Infections
- Brain damage resulting from trauma or poor blood flow to the brain
- Brain tumours
- Encephalitis (inflammation of the brain)
- Electrolyte problems
- Stroke
How is epilepsy in dogs and cats diagnosed?
The vet may suspect epilepsy if the animal experiences at least two unprovoked seizures more than 24 hours apart. Bearing in mind that in most cases the animal has recovered by the time she reaches the examination table, the vet will require a history of the onset of symptoms, number and duration of seizures, and other relevant information such as medications or poisons the animal may have ingested. A complete physical and neurological examination will be performed.
Two important factors in the diagnosis of epilepsy are the age at onset and the type and frequency of the seizures. If the animal has more than two seizures within the first week of onset, the veterinarian will probably rule out idiopathic epilepsy. Additionally, known causes of seizures, such as certain diseases, must be eliminated.
The diagnosis should be based on the medical history, neurological examination and laboratory tests (blood and/or urine). Further testing, such as imaging the brain using MRI and analysing the cerebrospinal fluid, may be recommended to detect structural abnormalities that could be causing the seizures.
Although there is no specific test to make a definite diagnosis, the following tests may be used to gain a greater understanding:
- Complete blood count, to look for infection, inflammation, anaemia and other blood-related conditions
- Biochemical profile, to assess liver, kidney and pancreatic function, sugar levels and electrolytes
- Urinalysis
- Thyroid screen
- Ultrasound
- Antigen testing for certain infections
- CT or MRI scans (imaging studies of the brain)
- Parasite checks
- Cerebral spine fluid (CSF) analysis to check for encephalitis (inflammation of the brain)
- Bile acid test to analyse liver performance
- In cats, testing for viruses such as feline leukaemia and feline AIDS
Prognosis
Epilepsy is typically a chronic disease requiring life-long treatment and care. Although early treatment and proper care are vital to for the animal’s general health and wellness, treatment will not necessarily eliminate seizures entirely.
The more seizures an animal experiences, the greater the likelihood of damage to the neurons in the brain and the more likely she is to have subsequent seizures. Younger dogs are more at risk for severe forms of certain types of epilepsy, including primary and idiopathic epilepsy, and they also tend to suffer more severely.
Treatment for epilepsy in dogs and cats
In most cases, epilepsy in dogs and cats cannot be cured. The ultimate goal of treatment is to maintain a seizure-free status without causing intolerable side effects. This balance is achieved in 15-30% of dogs.
Medical (drug) treatment
Antiepileptic drug (AED) therapy is effective in reducing the frequency of seizures for some animals. Corticosteroid medications and anti-convulsant medications may also help to reduce the frequency of seizures. The type of medications given will depend on the type of epilepsy the animal has, as well as other underlying health conditions.
The aim of AED treatment is to improve the quality of life by minimising the frequency and severity of attacks. Additionally, the prescribed medications should not cause serious side effects. Common side effects include tiredness, unsteadiness, increased appetite and thirst, drooling, vomiting, diarrhoea, weakness of the back legs, weight gain, excitability, restlessness and other behavioural changes.
AED treatment is generally considered to be successful if the frequency of seizures is reduced by at least half. Treatment may continue indefinitely, in most cases for the rest of the animal’s life, with periodic health checks and blood tests to ensure correct drug dosage, treatment efficacy and minimal side effects.
Other treatment options
Most of the treatment for animals with epilepsy is outpatient; however, in some cases certain medical procedures may be required, including surgery to remove tumours that may contribute to seizures. Seizures that are caused by lead poisoning, low blood sugar or certain infections, for example, can be stopped by treating the underlying cause.
In cases where the underlying cause cannot be treated, treatment is more about managing the severity and frequency of seizures (for example, a head trauma which caused brain damage or an inoperable tumour), anti-convulsant medications may be helpful.
Ongoing maintenance and treatment:
- It is recommended that animals stay indoors for a while (until the condition is stabilised) as seizures are likely to reoccur.
- Medications to be administered as directed by the vet.
- Regular follow ups with the vet will be required to see if medications are working with no serious side effects.
- Keep a detailed and accurate seizure diary or use an app which allows owners to track seizures on their smart phones (this will help determine if AED treatment is working).
- You may need to maintain the animal on a particular diet and provide meals at the same time each day, as changes can affect the blood levels.
What to do in event of a seizure:
- Stay calm if possible
- Move furniture or other nearby objects away, or if not possible, slide the animal away from any hazards such as a swimming pool or stairs
- Place pillows or blankets around the animal’s head and back
- Stay away from the animal’s mouth and head (do not put anything in the animal’s mouth)
- Keep other animals away
- Time the seizure if possible
- Be observant of, record or video the animal’s symptoms
- If the seizure continues for more than a few minutes, there is a chance the animal could overheat. Turn a fan on and bathe the paws in cold water.
- Talk gently to the animal for reassurance
- Do not touch the animal as she may unwittingly bite
- Call the vet at the end of the seizure for further instructions.
In summary
Seizures occur when abnormal electrical activity in the brain cause neurons in the brain to “misfire”. An epileptic seizure is characterised by the loss of voluntary control, often exhibited by convulsions (jerking or shaking movements and muscle twitching). Some seizures only effect a small part of the body, for example the face, while others can affect the entire body.
Epilepsy may have no known cause, can have a genetic basis or it can result from an injury to the brain or chemical imbalance. There are no specific diagnostic tests for epilepsy, but structural abnormalities in the brain can be confirmed by either MRI and/or cerebrospinal fluid analysis. If the dog or cat has repeated seizures over time, the diagnosis is likely to be epilepsy.
Treatment is mainly by means of drug therapy. In many cases, these drugs cannot completely eliminate the seizures without causing intolerable side effects. Therefore some animals will continue to experience seizures, although at a reduced rate, for the remainder of their lives.
Bow Wow Meow Pet Insurance can help protect you and your pet should an unexpected trip to your vet occur.
- Find out more about our dog insurance options
- Find out more about our cat insurance options
- Get an instant online pet insurance quote
Bow Wow Meow is proud to have been awarded winner of Canstar’s ‘Most Satisfied Customers’ Award in the Pet Insurance category for both 2024 and 2025!
Bow Wow Meow is proud to be the only Pet Insurer that has been awarded Product Review’s Top Rated Pet Insurance every year from 2018 to 2026! This is based on 3,193 independent customer reviews (as at 09/04/2026), with an overall rating of 4.5 stars.

We also have the following ratings on other review platforms:
Google Review rating of 4.5 stars (based on 1,358 reviews)
Trust Pilot rating of 4.6 stars (based on 555 reviews)
Bow Wow Meow has been chosen as Winner of 4 categories in the 2026 Finder Pet Insurance Customer Satisfaction Awards!
– Most Trusted Pet Insurance
– Easiest to Claim Pet Insurance
– Most Recommended Pet Insurance
– Legendary Service Pet Insurance
We also received Highly Commended Awards for Loved Brand Pet Insurance and Best Value Pet Insurance.
Bow Wow Meow is an Australian-owned and operated pet insurance provider. Our focus is purely on pets, and we are proud to have helped provide peace of mind to over 200,000 Aussie pet owners since 2008.
More information
- https://pets.webmd.com/dogs/dog-seizure-disorders#1
- https://www.petmd.com/dog/conditions/neurological/c_dg_seizures_convulsions
- https://www.thekennelclub.org.uk/health/for-owners/epilepsy/
- http://www.pethealthnetwork.com/dog-health/dog-diseases-conditions-a-z/canine-epilepsy
- https://www.australiandoglover.com/2015/11/seizures-and-epilepsy-in-dogs-causes.html
- https://www.petmd.com/cat/conditions/neurological/ct_epileptic_seizures%20