Hyperadrenocorticism (Cushing’s disease) in dogs
What is hyperadrenocorticism in dogs?
Hyperadrenocorticism, or Cushing’s disease, is one of the most common endocrine disorders that affects dogs. The endocrine system is made up of the glands that produce hormones, which are used for a wide range of functions, such as metabolism, respiration, reproduction and mood.
Hyperadrenocorticism is characterised primarily by overproduction of the hormone cortisol. Cortisol is a hormone that is produced in the adrenal glands. Cortisol performs many useful functions in the body, such as responding to stress and moderating the immune system. However, excessive cortisol in an animal’s body can do a lot of damage and may be life-threatening. It usually develops in middle-aged to older animals (7 to 12 years old). The disease is often insidious and slowly progressive.
What are the symptoms of hyperadrenocorticism in dogs?
The symptoms of hyperadrenocorticism are brought on primarily by the chronic excess of cortisol in the body. These symptoms are common to many diseases and conditions, so do not necessarily indicate the presence of hyperadrenocorticism.
The most common symptoms associated with hyperadrenocorticism in dogs include:
- an increase in hunger and appetite; polyphagia
- an increase in thirst and water consumption; polydipsia
- an increase in urination; polyuria
- increased or excessive panting
- heat intolerance
- a bloated, pot-bellied abdomen
- truncal obesity
- fat pads on the neck and shoulders
- lethargy, lack of energy or lack of activity
- decline in coat quality
- recurrent infections, such as skin, ear, urinary tract
- insomnia
- muscle weakness, loss of muscle
- skin problems – alopecia, especially truncal, darkening, blackheads, thinning, bruising
- hard white scaly patches on the skin and elbows
- neurologic abnormalities in advanced cases of the disease – circling, behavioural changes, seizures, anorexia
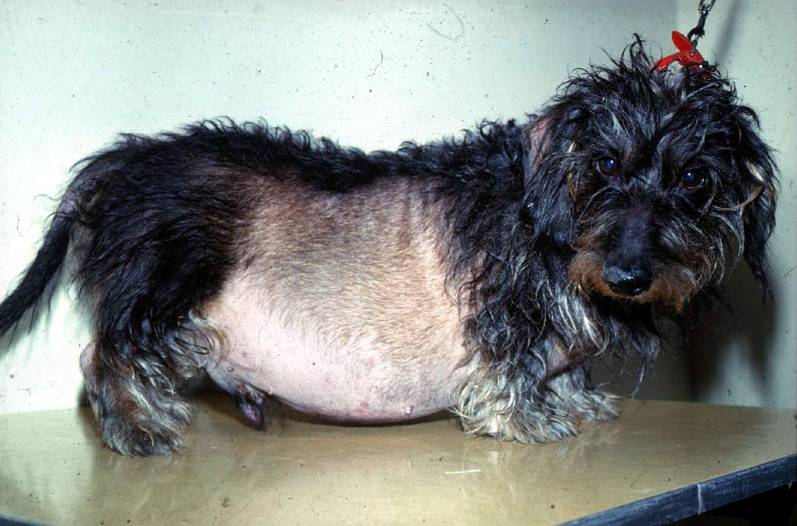
Dog with hyperadrenocorticism (cushing’s disease)
Source: https://animalendocrine.blogspot.com/2011/03/cushings-syndrome-common-hormonal.html
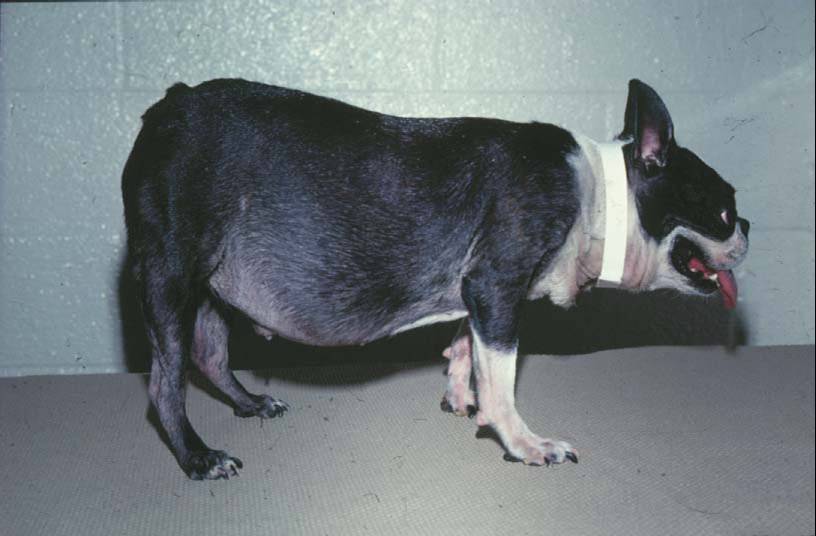
Dog with hyperadrenocorticism (cushing’s disease)
Source: https://animalendocrine.blogspot.com/2011/03/cushings-syndrome-common-hormonal.html
What is the cause of hyperadrenocorticism in dogs?
There are three routes by which hyperadrenocorticism can occur. While the symptoms are essentially the same, it is important to identify the specific cause, because the treatments and prognoses are different for each of these.
Pituitary gland tumour – Pituitary-dependent hyperadrenocorticism (PDH)
In pituitary-dependent hyperadrenocorticism, a tumour of the pituitary gland causes excessive production of adrenocorticotropic hormone (ACTH). The pituitary gland is located within the brain. ACTH is a hormone produced by the pituitary gland that stimulates the adrenal glands to release cortisol into the body. This is the most common cause of hyperadrenocorticism – around 80 to 85% of all cases in dogs.
Breeds in which PDH is commonly seen include Miniature Poodles, Dachshunds, Boxers, Boston Terriers, and Beagles.
Adrenal gland tumour – Adrenal-dependent hyperadrenocorticism (ADH)
In adrenal-dependent hyperadrenocorticism, a tumour of the adrenal gland causes an excessive production of cortisol. The adrenal glands are two endocrine glands that sit on top of each kidney. Most of the cortisol in the body is produced by the adrenal glands. If there is a tumour present, the adrenal gland will secrete an excess of cortisol.
In around 15 to 20% of cases, usually in larger breeds, hyperadrenocorticism is the result of a tumour of the adrenal gland, and there is a clear predilection in females (3:1).
Iatrogenic hyperadrenocorticism
Iatrogenic hyperadrenocorticism results from chronic, excessive use of corticosteroid medications. These medications may be administered orally or by injection, and may be prescribed in order to treat allergies, immune disorders and certain types of cancer, to reduce inflammation or as replacement therapy for low cortisone levels.
In the case of iatrogenic hyperadrenocorticism, although these medications were prescribed for an appropriate medical reason, their use is now detrimental as they are causing an excessive amount of cortisol in the body.
How is hyperadrenocorticism in dogs diagnosed?
Hyperadrenocorticism can be a difficult disease to diagnose and confirm. There is no single test or combination of tests that is completely accurate for diagnosing it. However, the testing process is critically important in order to determine the best treatment options and prognosis for your dog.
The first steps the vet will take are a comprehensive health history and a complete physical examination. These will most likely be followed by lab work such as:
- blood chemistry profile
- complete blood count
- faecal examination
- urinalysis
If the results of these tests lead your vet to suspect hyperadrenocorticism, a combination of the following tests will follow to definitively diagnose it and identify which type it is:
Urine cortisol:creatinine ratio (UCCR)
- The result is usually significantly elevated in dogs with hyperadrenocorticism
- If the results are normal (negative), hyperadrenocorticism is unlikely
- If the results are elevated, further testing is indicated, as many conditions can cause an elevated result.
Low dose dexamethasone suppression test (LDDS): The most common test used to diagnose hyperadrenocorticism, which in simplified terms works as follows:
- A blood sample is taken to measure the baseline cortisol level
- A small amount of dexamethasone is injected into the dog (dexamethasone inhibits cortisol secretion in normal dogs)
- Blood cortisol levels are measured four and eight hours later
- If there is no decrease in cortisol levels, hyperadrenocorticism is indicated.
ACTH Stimulation Test: Another commonly used test to diagnose hyperadrenocorticism
- Adrenocorticotropic hormone (ACTH) is a hormone produced by the pituitary gland that stimulates the adrenal glands to release corticosteroids.
- Levels of ACTH are increased in pituitary-dependent hyperadrenocorticism (PDH); therefore measurement of ACTH concentrations is the most reliable way to discriminate between PDH and ADH.
High-dose dexamethasone suppression test (HDDS)
- This test is used to differentiate between PDH and ADH
- In dogs with PDH, the administration of a high dose of dexamethasone will suppress ACTH and, hence, cortisol secretion.
Diagnostic imaging
- Abdominal ultrasound may be used to:
- to determine adrenal gland size
- to investigate the presence of any unusual tissue
- guide a biopsy to determine if the tissue is cancerous
- CT or MRI imaging may also be used to determine the presence of a pituitary gland tumour
- When a tumour has been diagnosed, diagnostic imaging can be used to examine the body for any metastatic spread of the disease.

What is the treatment for hyperadrenocorticism in dogs?
Treatment options depend greatly on the type of hyperadrenocorticism as well as the severity of the symptoms. If the symptoms are not too serious, treatment may not be necessary unless they worsen over time.
Pharmacological treatments aim to reduce the secretion of cortisone from the adrenal gland or pituitary gland by reducing the activity of these glands.
Iatrogenic (over-use of corticosteroid medication)
Treatment is relatively straightforward, requiring the discontinuation of the corticosteroid medication that is being administered. Your dog must be slowly weaned off the medication under your vet’s care so that complications associated with the discontinuation of the medication do not occur. Monthly ACTH stimulation tests may be performed to determine when steroid treatment can be withdrawn. Discontinuing these medications too quickly can lead to a life-threatening condition called Addisonian crisis, where the adrenal glands do not produce enough cortisol for normal function.
Unfortunately, this treatment usually results in the recurrence of the disease for which the corticosteroid was prescribed. Because there may have been adverse effects on the adrenal glands, treatment of this condition may also be required.
Adrenal Tumour
Adrenal tumours have a fifty percent chance of being malignant. Medical treatment of adrenal tumours is difficult, because they tend to be resistant to the medication.
If the tumour has not spread into surrounding structures or other organs, surgery is usually the treatment of choice. Surgical removal of a benign adrenal tumour (along with the adrenal gland) may cure the disease and the dog may return to normal health. The dog may be given a medication for a few months to shrink the tumour, prior to surgery to remove it.
Hypoadrenocorticism can occur immediately after surgical removal of the adrenal gland tumour when the levels of cortisone in the body are insufficient for normal functioning.
If the tumour has already spread then surgery may not be possible and the prognosis is less optimistic. If surgery is not an option, medication may have some benefit in managing the disease.
Pituitary Tumour
The pituitary gland tumour may range in size from microscopic to large and it may be either benign (non-spreading) or malignant (metastasising), but in most cases of PDH it is benign.
Treatment usually comprises medication which suppresses cortisol production. This medication will need to be taken for the rest of the animal’s life. Your dog may experience adverse side effects, so close monitoring of your dog’s condition is essential to determine when treatment will be beneficial. If symptoms are mild, treatment may not be required initially.
Treatment should commence where symptoms are more severe or potentially dangerous, such as:
- High blood pressure
- Recurrent infections
- Increased urine protein:creatinine ratio, which signals kidney problems
- Excessive urination and urinary accidents
If your dog does have an adverse reaction to the medication, contact your vet immediately. Other drugs may be prescribed to combat the reaction.
Signs of an adverse reaction are:
- lack of energy
- weakness
- lack of appetite
- vomiting
- diarrhoea
- difficulty walking
Generally, if the activity of the adrenal gland can be controlled with medication and close medical supervision, many dogs with PDH can live normal lives for many years. The goal is to suppress cortisol production enough to keep the animal healthy, but not so much that the opposite problem occurs — hypoadrenocorticism, or Addison’s disease. Therefore, close monitoring of dogs undergoing drug treatment for PDH is essential.
In some cases of PDH, radiation of the pituitary tumour may be indicated, such as when neurological symptoms are evident, for example seizures, anorexia, circling, behavioural changes, or when a large pituitary tumour is observed.
Radiation therapy can have a high success rate in shrinking the tumour. Medication will usually be required for several months after radiation until residual ACTH secretion ceases, and it may take some months before the signs of PDH subside. The long-term outcome is good because radiation therapy has a low morbidity rate and it targets the primary cause of the disease, the pituitary tumour itself.
Overview
Hyperadrenocorticism is either naturally occurring, where the dog’s own body overproduces cortisol, or when it consumes corticosteroid medications at high doses and/or over a long period of time. It is an insidious endocrine disease that will often quietly affect the body systems for a long time, causing damage but without any defining symptoms. Some of the more common symptoms are increases in thirst, appetite, urination and panting and a pot-bellied abdomen.
There are three mechanisms by which this disease can occur. It is important to identify the type of hyperadrenocorticism because each is treated differently and each has a different prognosis. With early diagnosis, appropriate treatment and ongoing medical care, the disease can be successfully managed; however, it is infrequently cured.
Bow Wow Meow Pet Insurance can help protect you and your dog should an unexpected trip to the vet occur.
-
Find out more about our dog insurance options
-
Get an online pet insurance quote
Bow Wow Meow is proud to have been awarded winner of Canstar’s ‘Most Satisfied Customers’ Award in the Pet Insurance category for both 2024 and 2025!
Bow Wow Meow is proud to be the only Pet Insurer that has been awarded Product Review’s Top Rated Pet Insurance every year from 2018 to 2026! This is based on 3,193 independent customer reviews (as at 09/04/2026), with an overall rating of 4.5 stars.

We also have the following ratings on other review platforms:
Google Review rating of 4.5 stars (based on 1,358 reviews)
Trust Pilot rating of 4.6 stars (based on 555 reviews)
Bow Wow Meow has been chosen as Winner of 4 categories in the 2026 Finder Pet Insurance Customer Satisfaction Awards!
– Most Trusted Pet Insurance
– Easiest to Claim Pet Insurance
– Most Recommended Pet Insurance
– Legendary Service Pet Insurance
We also received Highly Commended Awards for Loved Brand Pet Insurance and Best Value Pet Insurance.
Bow Wow Meow is an Australian-owned and operated pet insurance provider. Our focus is purely on pets, and we are proud to have helped provide peace of mind to over 200,000 Aussie pet owners since 2008.
More information
https://www.vetwest.com.au/pet-library/cushing%E2%80%99s-disease-in-dogs-hyperadrenocorticism
https://www.petmd.com/dog/conditions/endocrine/c_dg_hyperadrenocorticism
https://www.petmd.com/blogs/fullyvetted/2012/june/confusion_with_cushings_disease-24744









