Osteoarthritis in dogs
What is osteoarthritis in dogs?
The most common form of arthritis in dogs is osteoarthritis, also known as “OA”, rheumatism or degenerative joint disease (DJD). Normal joints have a layer of cartilage which acts as a cushion between the bones and provides a smooth surface for the adjoining bones to slide over freely. Osteoarthritis refers to the gradual and permanent deterioration of the smooth cartilage surface of the joints. The loss of joint cartilage results in less smooth movement of the bones, inflammation, thickening and stiffening of the joint, and often new bone formation around the joint (osteophytosis).
Osteoarthritis in dogs often develops slowly and may be well advanced before pain sets in. Since cartilage has no nerve supply, the joint disease may advance for some time without outward indications. As the disease progresses, bone spurs and thickening of the tissue around the joint can occur, causing more pain and stiffness.
Older dogs, large breeds, athletic and working dogs are at highest risk of developing osteoarthritis, as well as dogs that have hip or elbow dysplasia.
Cost of osteoarthritis treatment for dogs
According to Petsure data from 2024, osteoarthritis was the seventh most common condition claimed for in dogs overall, and the most common claim for dogs over eight years old.
The average and highest costs of treatment in 2024 for osteoarthritis were as follows:
| Claims data for osteoarthritis | Average cost of treatmentØ | Highest cost of treatmentØ |
| Dogs (all ages) | $823 | $39,289 |
| Dogs 8+ years old | $831 | $21,936 |
ØBased on PetSure claims data, 2024 calendar year. Reimbursement for these claims under a pet insurance policy would be subject to limits, such as annual benefit limits or sub-limits, benefit percentage, applicable waiting periods and any applicable excess. Cover is subject to the policy terms and conditions. You should consider the relevant Product Disclosure Statement or policy wording available from the relevant provider. Please note that values calculated are based on all claims for that condition and medically related conditions in each calendar year.
Because it is difficult to predict the costs of veterinary care, it can help to have measures in place to help prepare for the unexpected. Pet insurance can help by covering a portion of the eligible vet bill if the unexpected does happen.
Get a quote for 2 months free pet insurance for your puppy or kitten in their first year.
Symptoms of osteoarthritis in dogs

Many of the early symptoms of osteoarthritis in dogs are subtle and gradual behavioural changes, such as a decreased activity level. Unfortunately, the more obvious signs, like limping, may only occur in the end stages of long-term joint degeneration. The signs usually become more obvious as the osteoarthritis progresses and the pain worsens.
The symptoms of osteoarthritis are often non-specific, and can be caused by other conditions, or be mistaken for normal signs of ageing. These may include:
- A noticeable decrease in activity, and a general slowing down
- Stiffness of movement after rest, which eases as the joint “warms up” with use
- Limping, or favouring a particular limb
- Difficulty or inability to get up with ease, particularly after sleep or rest
- Reluctance to exercise (and to walk, jump, play, climb stairs etc.)
- Spending more time lying down and sleeping
- Struggling to get in or out of the car, or jump down from furniture
- Showing signs of pain or soreness (wincing when touched; irritability; fatigue, etc.)
- Partial or complete lameness, or inability to walk (this can occur suddenly, typically after vigorous or unfamiliar types of exercise)
- Change in gait, such as stiff or rigid walking, or bunny-hopping
- Clicking, grating or popping noises from the joints during movement
- Loss of muscle mass and increased weakness of the affected limbs
- Lagging behind on walks
- Whimpering or yelping in pain
- Behavioural changes, such as being aggressive or withdrawn.
Causes of osteoarthritis in dogs
There are a number of potential causes of and contributing factors to osteoarthritis. Once triggered, osteoarthritis appears to be a self-perpetuating process with a gradual progression.
Common causes or triggers include:
Ageing
In older dogs, osteoarthritis is typically associated with the ageing process and gradual wear and tear on the joints. However, it is not an inevitable consequence of ageing, as not all dogs succumb to it.
Joint problems
Secondary osteoarthritis in dogs of any age can be triggered by another joint problem, such as:
- Hip dysplasia – abnormal development of the hip
- Elbow dysplasia – abnormal development of the elbow
- Joint disorders, for example, osteochondrosis, a condition in which the bone and cartilage develop abnormally so that a flap of cartilage develops within the joint
- Trauma to the joint, for example, dislocation of the kneecap or shoulder
- Hyperlaxity – an excessive looseness of the joints.
Breed susceptibility

- Larger breeds are more susceptible to different forms of skeletal disorders than smaller dogs.
- Inherited conditions such as hip dysplasia are commonly seen in large breeds such as German Shepherds, Golden Retrievers, Labrador Retrievers, Staffordshire Terriers, Alaskan Malamutes, Samoyeds, Old English Sheepdogs, Rottweilers, and Saint Bernards.
- Smaller breeds prone to hip dysplasia include Pugs and French Bulldogs.
Other contributing factors
- Excessive bodyweight and obesity increase the stress on the joints, possibly contributing to early onset osteoarthritis
- Size – generally, the larger the animal, the more likely they are to suffer from osteoarthritis
- Lack of exercise leads to loss of muscle mass and less support for the affected joints
- Post-operative complications from orthopaedic surgery
- Diabetes
- Prolonged steroid treatment.
How is osteoarthritis in dogs diagnosed?

While osteoarthritis in canines is usually identified from the signs and symptoms exhibited, some of these symptoms can be caused by other conditions. Therefore, it is important that your vet confirms the diagnosis of osteoarthritis by other means, usually a combination of medical history, physical examination and imaging with X-rays.
Medical history and physical examination
The vet will take a thorough history and ask specific questions regarding your dog’s condition. A gait analysis is performed to reveal any subtle lameness and stiffness of gait.
The affected joint or joints are assessed for:
- Discomfort or pain when the joint is manipulated
- Decreased range of motion
- An accumulation of joint fluid (effusion)
- Osteophytes (bone spurs)
- Muscle atrophy (wasting).
Radiography (X-rays)
Radiography, usually performed under sedation or anaesthesia, is the most utilised diagnostic tool for osteoarthritis in dogs. However, it is limited, in that the radiographic signs of osteoarthritis are fairly non-specific.
Radiography may be used to identify:
- Bony changes (osteophytosis) around the affected joint
- Hardening and thickening of bone beneath the cartilage
- A narrowed joint space
- Increased fluid within the joint
- Limited soft tissue changes such as swelling around the joint
- A sample of joint (synovial) fluid may be taken during radiography for laboratory analysis (in osteoarthritic joints the volume of fluid may be increased).
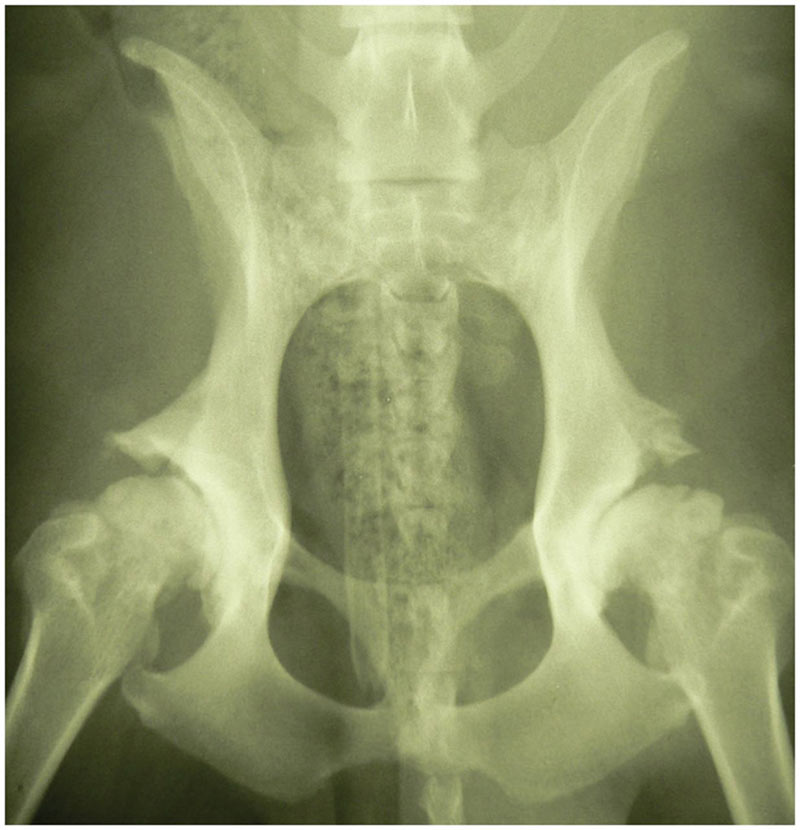
Ventrodorsal radiograph of the pelvis, demonstrating severe osteoarthritis in both coxofemoral joints. Source
Other diagnostic tools
- Magnetic resonance imaging (MRI) can provide useful information regarding soft tissue structures (ligaments, menisci).
- Computed tomography (CT) can be used to assess bony changes in complex joints such as elbows, carpi (wrists) or tarsi (ankles). This can be useful in the early stages of disease, as it may help to identify the primary lesion, which may not be present or obvious on radiographs.
- Blood work and urine samples to determine an older dog’s baseline health and to plan long-term medical therapy.
Prognosis
Osteoarthritis is a progressive disease that continues to worsen with time. The outlook for recovery depends on the location and severity of the joint disease. Appropriate treatment can slow down the progression of disease, ease the pain and improve quality of life. Many dogs can live comfortably for years following diagnosis.
Treatment for osteoarthritis in dogs
 Treatment for dog osteoarthritis has improved a great deal in the past few decades. However, there is presently no treatment that can cure or reverse the physical changes caused by degenerative joint disease in dogs, such as loss of cartilage and growth of bone spurs. Therefore, the main goals of treatment are to alleviate the pain and discomfort in the safest possible manner, and to prevent the condition from worsening, by minimising aggravation of the joint.
Treatment for dog osteoarthritis has improved a great deal in the past few decades. However, there is presently no treatment that can cure or reverse the physical changes caused by degenerative joint disease in dogs, such as loss of cartilage and growth of bone spurs. Therefore, the main goals of treatment are to alleviate the pain and discomfort in the safest possible manner, and to prevent the condition from worsening, by minimising aggravation of the joint.
The severity of the symptoms and how they affect your dog’s quality of life are the primary determinants of treatment. Based on your dog’s symptoms, age and overall health, your vet may use a combination of medical and surgical approaches, such as:
Exercise routine
- Consistent, daily low-impact activity is essential to help strengthen the muscles around the joint and promote joint stability
- Encourage moderate exercise that is easy on the joints, such as leash walking on flat, even ground
- Swimming is a non-weight bearing exercise that helps maintain muscle mass
- Avoid high impact and exuberant activities such as running, jumping or chasing balls
- If a flare-up occurs, reduce the duration and frequency of exercise, then slowly over a few weeks build back up to previous levels.
Weight management
- Excessive weight means extra pressure on the joints, which accelerates joint changes, increases discomfort and further limits mobility
- Reducing the dog’s body weight to an appropriate level will improve mobility and help minimise further joint damage
- A carefully monitored weight-loss regime, with regular weight checks, is recommended
- In many cases, medication can be reduced when an ideal weight is achieved.
Medication
Osteoarthritis is a long-term disease, and medical management should be aimed at the chronic pain associated with it and not just acute flare-ups. Medical treatment of osteoarthritis has vastly improved over the past few years, and medications are almost always a part of the treatment plan. Always use medications as directed by your vet, and be aware that long term medication can have unpleasant and potentially serious side effects.
Symptom-modifying drugs used to manage osteoarthritis generally aim to relieve the pain associated with the condition, and include:
- Non-steroidal anti-inflammatory drugs (NSAIDs), which are used to to ‘settle’ the joint and reduce pain and inflammation. These can have serious long-term effects, such as gastrointestinal problems, especially in geriatric dogs.
- Corticosteroids, which are administered to isolated joints by injection. These often provide rapid but short-lived alleviation of symptoms, and may need repeating once or twice (further repeats, as well as systemic steroid therapy, are not recommended as there can be detrimental side effects).
- Paracetamol/codeine – for pain management (not used in conjunction with NSAIDs)
- Oral opiates
- Pain relieving drugs designed to manage chronic pain
- Local intra-articular injections (in the joint) with different agents (corticosteroids, platelet-rich plasma, hyaluronic acid).
Nutritional joint supplements
- Glucosamine Chondroitin – a commonly prescribed joint supplement for dogs that have canine osteoarthritis. It lubricates the joints to allow for more fluid motion.
- Chondroitin sulphate – has been shown anecdotally to ease symptoms
- Omega-3-fatty-acids – research has shown that foods that provide high levels of eicosapentaenoic acid (EPA) can help decrease inflammation.
Surgery
If surgery is performed, recovery is usually very good, for example with total joint replacement surgery, where the diseased joint is completely removed and replaced. In other cases, surgery may help alleviate symptoms and slow the progression of the disease.
Surgical treatment options include:
- Removal of aggravating causes like bone or cartilage fragments
- Total joint replacement / arthroplasty (most commonly of the hips, also available for elbows and stifle)
- Arthrodesis (fusion of the joints, producing a rigid joint, so more suitable to the low motion joints such as the carpus and tarsus)
- Joint stabilization techniques
- Amputation (in extreme cases)
- Arthroscopy, a type of key-hole surgery using a camera, which may be used for direct visual examination of the inside of the affected joint and cartilage, removal of loose fragments or lesions, and joint stabilisation.
Environmental changes
- Purchase a comfortable, cushioned mattress or floor-level dog bed positioned away from drafts – this may help to lessen discomfort and stiffness
- Cover your dog with warm, soft blankets when sleeping or resting
- Turn on the heating or provide a jumper/coat to keep your dog warm during the cold winter months.
Additional treatment options and aids

- Massage – learn massage techniques and simple physical therapy
- Ramps – for climbing in and out of the car or up and down stairs
- Elevate food bowls to the appropriate level for larger dogs with back or neck stiffness
- Hydrotherapy – special tanks filled with warm water that have a treadmill on the bottom – the warmth of the water helps to alleviate pain and the level of the water helps to support the weight of the dog as the treadmill moves
- Acupuncture – small needles are inserted in to areas of inflammation and pain for a period of time, usually between 10 and 30 minutes. This is frequently used for elderly pets or pets that are not suited to medications that could cause organ damage or sickness.
- Ultrasound therapy
- Laser therapy
- Application of cold and heat to relieve joint pain.
Prevention
Unfortunately, osteoarthritis and other forms of degenerative bone disease cannot be prevented from occurring. However, by modifying your dog’s diet and exercise regimen and providing medication and supplements recommended by your vet, can lessen the severity of the symptoms and decrease the progression of the disease.
In conclusion
Osteoarthritis is a degenerative joint disease that is defined as the progressive and permanent deterioration of the cartilage surrounding the joints of the body. It results in chronic joint inflammation, and in many cases, pain and discomfort, that can potentially be crippling to the dog. Canine osteoarthritis is one of the most common disease among dogs, particularly older ones.
Symptoms may include a stiff gait, reluctance to exercise, trouble getting up and down, muscle loss and weakness, and trouble executing steps or stairs. Treatment options to consider once a diagnosis of osteoarthritis is made include surgery, medications, and a weight loss plan. It is important to avoid trauma or excessive pressure to the joints. Consult your veterinarian if you think your dog may be exhibiting the signs of osteoarthritis.
More information
https://www.acvs.org/small-animal/osteoarthritis-in-dogs
https://www.caninejournal.com/canine-osteoarthritis/
http://www.theveterinaryexpert.com/arthritis/osteoarthritis-in-dogs/
https://wagwalking.com/condition/osteoarthritis
https://www.petmd.com/dog/conditions/musculoskeletal/c_multi_arthritis_osteoarthritis
https://canna-pet.com/osteoarthritis-dogs/
Bow Wow Meow Pet Insurance can help protect you and your dog should an unexpected trip to the vet occur.
-
Find out more about our dog insurance options
-
Get an online pet insurance quote
Bow Wow Meow is proud to have been awarded winner of Canstar’s ‘Most Satisfied Customers’ Award in the Pet Insurance category for both 2024 and 2025!
Bow Wow Meow is proud to be the only Pet Insurer that has been awarded Product Review’s Top Rated Pet Insurance every year from 2018 to 2026! This is based on 3,193 independent customer reviews (as at 09/04/2026), with an overall rating of 4.5 stars.

We also have the following ratings on other review platforms:
Google Review rating of 4.5 stars (based on 1,358 reviews)
Trust Pilot rating of 4.6 stars (based on 555 reviews)
Bow Wow Meow has been chosen as Winner of 4 categories in the 2026 Finder Pet Insurance Customer Satisfaction Awards!
– Most Trusted Pet Insurance
– Easiest to Claim Pet Insurance
– Most Recommended Pet Insurance
– Legendary Service Pet Insurance
We also received Highly Commended Awards for Loved Brand Pet Insurance and Best Value Pet Insurance.
Bow Wow Meow is an Australian-owned and operated pet insurance provider. Our focus is purely on pets, and we are proud to have helped provide peace of mind to over 200,000 Aussie pet owners since 2008.











