Cataracts in dogs and cats

Summary
A cataract is an opacity of the lens that prevents light from reaching the retina, leading to vision impairment. Cataracts can develop in one or both eyes and they may progress slowly or rapidly, leading to vision impairment and/or blindness. There are a variety of causes of cataracts in dogs and cats, including genetics, age, trauma and metabolic diseases such as diabetes. Cataract removal has a high rate of success and a good prognosis, with sight often restored to near normal. However, not all dogs and cats with cataracts are candidates for surgery, and a conservative approach may be taken to their management.
What are cataracts in dogs and cats?
The eye is a complicated organ comprised of several structures that work together to enable vision. One of these is the lens – a soft, clear structure which functions as a focusing device by ‘bending’ incoming light rays to focus on the retina at the back of the eye. The lens is made up of water and protein and is held in place by tissue fibres located just inside the pupil. Cataracts are formed when protein strands in the lens clump together, causing an area of cloudiness or opacity.
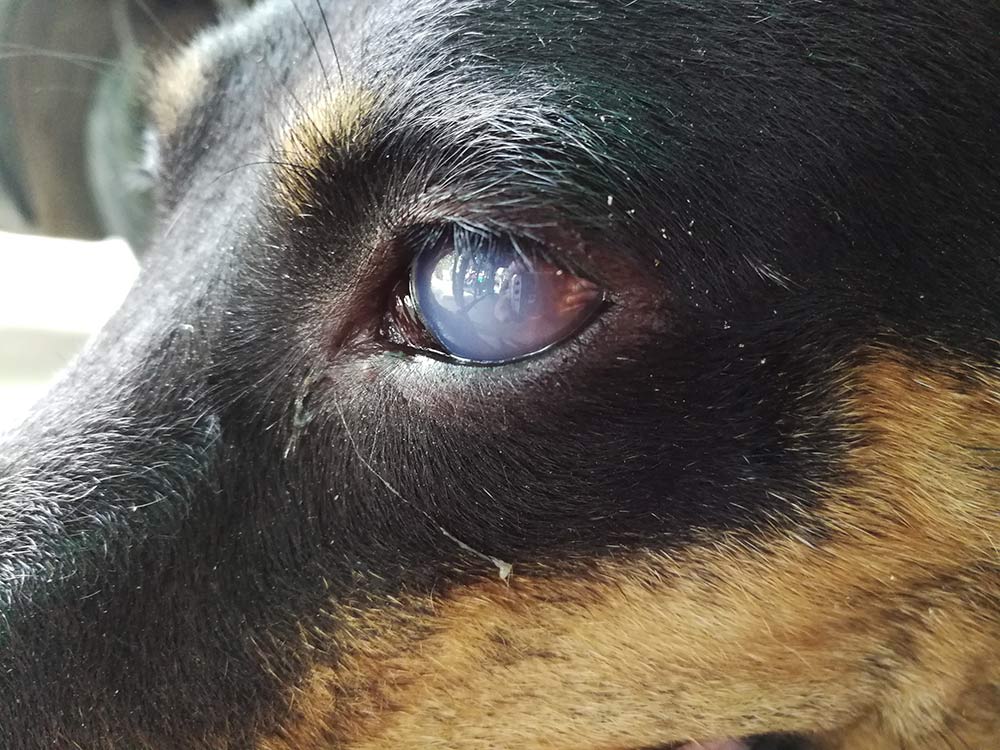
The lens is transparent so that light can pass through. Cataracts impair this function; they block light from reaching the retina. Cataracts may initially affect only a small part of the lens – these are called immature cataracts – but generally they progress to affect more of it over time. If the entire lens is opaque, the cataract is termed mature. The eye cannot see through the portion of the lens where there is a cataract, so if the entire lens is affected, the eye will be blind.
While cats can develop cataracts, dogs are thought to suffer from cataracts more commonly than any other species. However, cloudiness of the eye in dogs does not always mean there is a cataract. In young dogs, cataracts are sometimes confused with the minor lens imperfections, and in older dogs, with the normal increase in the thickening and hardening of lens tissue. Lenticular or nuclear sclerosis is a normal aging process in which the lens in dogs over 7 years of age develops a whiter or blue-greyish haze, mimicking the appearance of a cataract. This phenomenon does not seem to impair vision, and a veterinarian can easily distinguish it from cataracts.
Cost of managing a cataract condition for dogs and cats
Managing a cataract condition can range from basic medical treatment to surgery. According to PetSure Claims data 2022, the average claimed cost of cataract management was $1,805Ø while the average claimed amount for cases that required surgery was $7,079Ø. Pets that require cataract surgery are more likely to be over the age of 8 years old.
ØBased on PetSure claims data, 2022 calendar year. Reimbursement for these claims under a pet insurance policy would be subject to limits, such as annual benefit limits or sub-limits, benefit percentage, applicable waiting periods and any applicable excess. Cover is subject to the policy terms and conditions. You should consider the relevant Product Disclosure Statement or policy wording available from the relevant provider. Please note that values calculated are based on all claims for that condition and medically related conditions in each calendar year.
Because it is difficult to predict the costs of veterinary care, it can help to have measures in place to help prepare for the unexpected. Pet insurance can help by covering a portion of the eligible vet bill if the unexpected does happen.
Get a quick quote
Symptoms of cataracts in dogs and cats
Because dogs and cats can use their keen senses of hearing and smell to compensate for loss of vision, it can be difficult for a pet owner to detect cataracts at an early stage. Symptoms, when they do occur, tend to relate to the degree of vision impairment. For example, dogs with less than 30 percent lens opacity often display few or no symptoms, whereas those with greater than 60 percent opacity of the lens may have difficulty seeing in dimly lit areas.
Symptoms relating to the eyes may include:
- A cloudy or white / grey / bluish appearance
- Having difficulty seeing in bright light
- Having difficulty seeing in dim light
- Eye irritation/redness, discharge or blinking
- Rubbing or scratching of the eyes
- Whiteness in the pupils

Behavioural signs in dogs:
- Increasingly cautious in their movements
- Tend to stay closer than usual to their owner
- A sudden reluctance to climb stairs or jump on furniture
- Clumsiness, e.g., bumping into familiar furniture
- Difficulty catching or obtaining food, e.g., sniffing for treats rather than seeing them
- Unable to fetch or retrieve as well as previously
Behavioural signs in cats:
- Less agile
- Bump into familiar furniture
- Appear to have difficulty finding its food bowl or litterbox
- Reluctant to move about in unfamiliar places
- Tentative and cautious going up and down stairs
Causes of cataracts in dogs and cats
Cataracts can be congenital (born with the condition) or acquired (occurring later in life). There are a variety of causes and risk factors contributing to the development of cataracts, including:
- Genetics (inherited)
- Age-related
- Trauma / injury
- Inflammation
- Metabolic diseases, particularly diabetes mellitus
- Malnutrition
- Exposure to radiation or toxic substances
Genetics
A very common cause is genetics, with many breeds known to have a genetic predisposition to developing cataracts. Hereditary cataracts tend to form at a young age, between 1 to 5 years old. Breeds commonly affected by hereditary cataracts include:
- Australian Shepherds
- American Cocker Spaniels
- Siberian Huskies
- Staffordshire Bull Terriers
- Standard Poodles
- Miniature Schnauzers
- Golden Retrievers
- Labrador Retrievers
- Boston Terriers
- French Bulldog
In cats, most cases of cataracts are also inherited, with Persians, Birmans, and Himalayans all predisposed to cataracts.
Young age
Juvenile cataracts are fairly rare. They develop during puppyhood, usually between 6 months and 6 years of age. There may be a genetic component to developing juvenile cataracts in certain breeds.
Old age
Most cataracts in dogs develop with age, as a result of natural age-related degeneration within the structure of the lens. Many dogs older than 8 years will develop some degree of cloudiness to the lens of the eye. In cats, age is not generally the key factor.
Diabetes
Diabetic dogs are especially susceptible to developing cataracts. In this condition, as the blood sugar soars, so does the sugar level of the fluids within the eye that nurture the lens. The excess sugar is absorbed by the lens and transformed into sorbitol. Sorbitol within the lens draws water into the lens, causing an irreversible cataract in each eye.
Cataracts are practically unavoidable in diabetic dogs no matter how good their insulin regulation is; however, diabetic cats have a different method of sugar metabolism in the eye and do not acquire cataracts from diabetes.
Trauma and infection
Cats most often develop cataracts secondarily to inflammation resulting from eye trauma, viral infection or other infections. The most common underlying cause of cataracts in cats is uveitis, an inflammation of the middle layer of tissue in the eye wall. Traumatic injury that results in a perforated lens (e.g., as a result of a fight with another cat) and experiencing an electric shock can also lead to the development of a cataract.
Nutrition
Poor nutrition as a puppy or kitten, resulting in a dietary deficiency. However, cataracts resulting from poor nutrition are rare nowadays because of modern advances in diets for pets.
Idiopathic
In some cases, the cataract is idiopathic, which means the cause cannot be identified.
How are cataracts in dogs and cats diagnosed?
Sometimes cataracts do not pose any additional problems beyond vision loss, but other times they can lead to an even more serious issue — glaucoma (increased pressure within the eye). Therefore, if you observe cloudiness or other changes in one or both of your pet’s eyes, you should consult your veterinarian immediately. Prompt diagnosis is important; while there is a surgical treatment for cataracts, it is usually best to do this as early in their formation as possible.
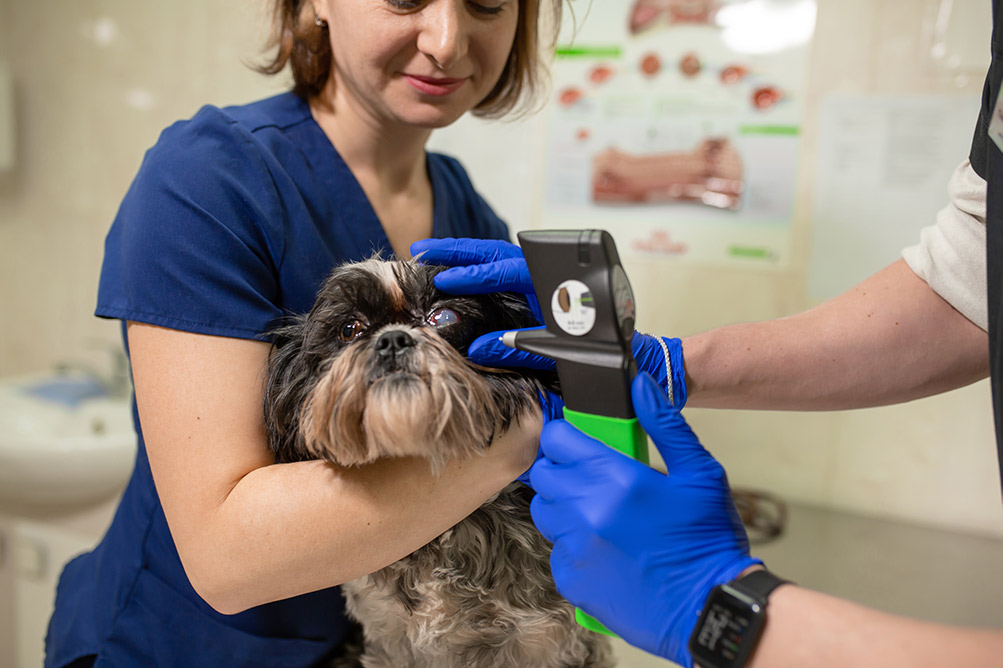
The vet will ask for a thorough history of your dog’s health, including the onset and nature of the symptoms, and possible underlying issues that might have caused the problem. He or she will then perform a complete physical examination, focusing on the eyes and ocular region, to determine the presence of cataracts and the severity of the problem.
Routine diagnostic tests may be conducted, such as complete blood count, biochemistry profile and urinalysis. However, the results of these tests are usually non-specific unless an underlying disease such as diabetes is detected.
Before surgery is considered, the retina must be assessed to rule out concurrent retinal degeneration. Your vet may refer you to a veterinary ophthalmologist to determine the extent of the problem and to establish whether your dog is a candidate for surgical cataract repair. Ultrasound (to look for retinal detachment) and electroretinography (to measure the functioning of the retina) are advanced diagnostic exams that can be used to ascertain the severity of the issue and may confirm whether surgery is an appropriate treatment. If the retina is functional, cataract surgery can restore vision; if the retina is non-responsive, there is no point in treating the cataract as vision cannot be restored.
The vet or specialist will also check the eye for uveitis or other inflammation, so that treatment can be administered before surgery, and eye drops may be required for a period.
Prognosis
Cataracts in dogs is typically a progressive disorder that, if not treated quickly, may lead to blindness in one or both eyes. However, the rate of progression depends on the location of cataract within the lens and the age of the animal, as well as any underlying cause of the cataract. The cataracts induced by diabetes in dogs are usually very rapid in their progress, while in some instances in young animals, cataracts disappear on their own and sight may be regained.
If surgery is recommended, it typically comes with a good prognosis and a high rate of success: Overall, a 95 percent vision rate is described immediately after cataract surgery with 80 percent having long-term vision success. However, surgery is not suitable for all animals with cataracts. Those with progressive cataracts that are not candidates for surgery can learn to adjust to their decreased vision and are usually able to compensate for the loss of vision with their keen senses of hearing and smell.
Treatment for cataracts in dogs and cats
Age itself is not a consideration when determining cataract treatment; of greater importance is the animal’s overall health, the stage of development of the cataract, and its underlying cause. Cataracts can have different behaviours depending on their origin. Your vet or specialist will determine the most appropriate course of action for your pet.
Because it is difficult to predict the costs of veterinary care, it can help to have measures in place to help prepare for the unexpected. Pet insurance can help by covering a portion of the eligible vet bill if the unexpected does happen.
Get a quote for 2 months free pet insurance for your puppy or kitten in their first year.
Surgical treatment
Treatment for cataracts in dogs often entails a procedure to remove the affected lens or lenses. Historically, removing the cataract meant surgically cutting into the eye and physically removing the lens. This technique may still be used for older animals whose lenses are compact. For younger patients in whom the lens is soft, a more modern technique called phacoemulsification is preferred.
Phacoemulsification involves the use of an ultra-sonic device to disintegrate, and then remove, the affected lens under anaesthetic. To ensure normal sight and prevent extreme farsightedness, after the lens is removed, an artificial lens is implanted. Phacoemulsification has shown a greater than 90 percent success rate in dogs and has become the most common method of removing cataracts.
If cataract removal is recommended by your veterinarian, it is advised not to delay. Surgical treatment is most likely to be successful when performed before cataract maturation is complete and before inflammation in the front chamber of the eye occurs. Particularly if a cataract is a type that can be expected to progress rapidly, such as the hereditary cataracts of young cocker spaniels, it is beneficial to pursue surgical treatment when the cataract is smaller and softer, as removal will be easier.
Conservative management
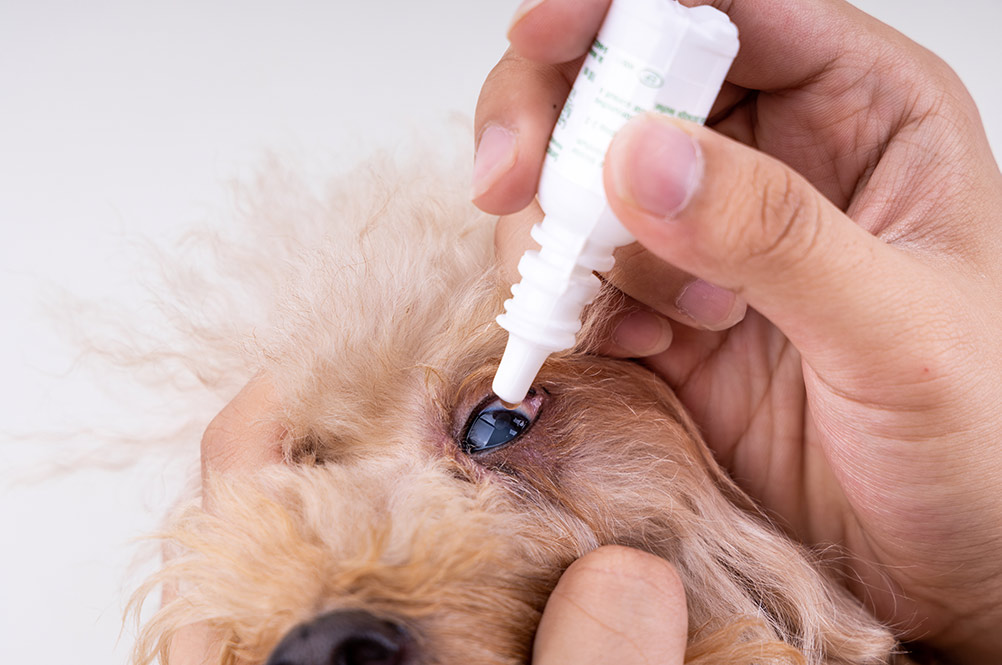
If the cataracts are small and do not impede the dog’s vision, the vet may recommend that they be left alone and regularly monitored for progression. Cataracts in only one eye are usually left alone and managed conservatively. Immature and incomplete cataracts may benefit from topical medication (eye drops) 2 to 3 times per week.
Congenital cataracts that are present at birth and juvenile cataracts in young animals may become less of a problem as the animal matures. The lens grows, while the cataract often remains the same size, allowing for some restoration of vision as the dog learns to compensate and see through the clear areas of the lens. Treatment may not be necessary unless the cataracts become problematic.
Surgery is often not recommended for dogs with non-hereditary forms of cataract, and particularly where there is inflammation of the eye. Additionally, surgery is not warranted if it is not likely to restore vision (such as where the retina is damaged). In animals in which surgery is not performed, continued monitoring is very important because complications such as glaucoma can occur.
Unsure how serious it is?
Bow Wow Meow policyholders can get access to trusted vet care anytime, anywhere, at no additional cost. Connect to an experienced Australian registered vet via video call, 24/7. Whether it’s providing vet advice, setting up at-home treatment plans, or confirming if you need to visit a vet in person, you can get help when you need it.
Find out more about our pet insurance cover options.
Treatment for cats
As for dogs, the treatment of cataracts in cats will depend upon their underlying cause, stage of development, and the overall health of the animal. Note that routine eye examinations as part of your cat’s annual check-up will help in monitoring her eye health, as will keeping vaccinations up to date, to help prevent viral infections that may predispose her to cataracts.
Treatment may include:
- Treating the underlying cause, if identified
- Eye drops to prevent inflammation and other secondary problems
- Surgical removal of the cataract, if the cat is otherwise healthy and is a suitable candidate for surgery
- If surgery is not performed, on-going monitoring by the vet for signs of glaucoma, uveitis and a blind, shrunken eye.
Bow Wow Meow Pet Insurance can help protect you and your pet should an unexpected trip to your vet occur.
- Find out more about our dog insurance options
- Find out more about our cat insurance options
- Get an instant online pet insurance quote
Bow Wow Meow is proud to have been awarded winner of Canstar’s ‘Most Satisfied Customers’ Award in the Pet Insurance category for both 2024 and 2025!
Bow Wow Meow is proud to be the only Pet Insurer that has been awarded Product Review’s Top Rated Pet Insurance every year from 2018 to 2026! This is based on 3,193 independent customer reviews (as at 09/04/2026), with an overall rating of 4.5 stars.

We also have the following ratings on other review platforms:
Google Review rating of 4.5 stars (based on 1,358 reviews)
Trust Pilot rating of 4.6 stars (based on 555 reviews)
Bow Wow Meow has been chosen as Winner of 4 categories in the 2026 Finder Pet Insurance Customer Satisfaction Awards!
– Most Trusted Pet Insurance
– Easiest to Claim Pet Insurance
– Most Recommended Pet Insurance
– Legendary Service Pet Insurance
We also received Highly Commended Awards for Loved Brand Pet Insurance and Best Value Pet Insurance.
Bow Wow Meow is an Australian-owned and operated pet insurance provider. Our focus is purely on pets, and we are proud to have helped provide peace of mind to over 200,000 Aussie pet owners since 2008.
Sources
“Cataracts Can Occur as Your Dog Ages”, AKC, https://www.akc.org/expert-advice/health/cataracts-can-occur-as-your-dog-ages/. Accessed 10 Mar 2026
“Cataracts in cats”, Pet Health Network, https://www.pethealthnetwork.com/cat-health/cat-diseases-conditions-a-z/cataracts-cats. Accessed 10 Mar 2026
“Cataracts in Dogs”, Pet Health Network, https://www.pethealthnetwork.com/dog-health/dog-diseases-conditions-a-z/cataracts-dogs. Accessed 10 Mar 2026
“Cataracts in Dogs and Cats”, Veterinary Partner, https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4951531. Accessed 10 Mar 2026
“Cataracts in Dogs: Signs, Causes, and Treatment”, petMD, https://www.petmd.com/dog/care/cataracts-dogs-everything-you-need-know. Accessed 10 Mar 2026
“Cataracts in Dogs: Signs, Causes and Treatment”, petMD, https://www.petmd.com/dog/conditions/eye/c_dg_cataract. Accessed 10 Mar 2026
“Cataracts in Cats: Signs, Treatment Options, & Surgery Cost”, petMD, https://www.petmd.com/cat/conditions/eye/c_ct_cataract. Accessed 10 Mar 2026
“Feline Cataracts”, Cornell Feline Health Center, https://www.vet.cornell.edu/departments-centers-and-institutes/cornell-feline-health-center/health-information/feline-health-topics/feline-cataracts. Accessed 10 Mar 2026










